Introduction to a Helpful and Trustworthy Parent Guide to Everything You Need to Know
Welcome to this authentic parent guide a forceps birth injury.
- Forceps delivery can be a safe, well-indicated assisted birth.
- It can also be frightening to process when forceps delivery complications arise, especially if your baby has bruising, unusual head or facial findings, feeding challenges, or concerns raised by clinicians.
- This guide explains what forceps are, why they are used, which injuries are possible, what to watch for, what care typically involves, and how to advocate effectively for your child in 2026 and beyond.
If your child suffered a forceps birth injury, and you suspect Forceps delivery medical malpractice, call Nashville forceps delivery complications lawyer Timothy L. Miles today to see if you qualify for a forceps delivery complications lawsuit, and potentially entitled to substandial compensation. The call is free and so the fee unless we win or settle you case so call today and and see what a Nashville forceps delivery complications lawyer can do for you. (855) 846-6538 or [email protected].

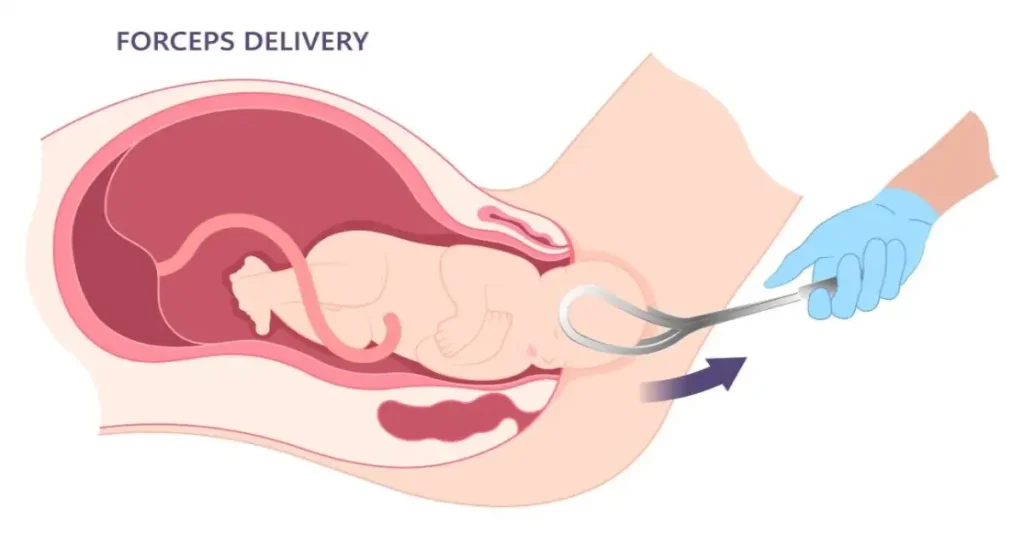
What a Forceps Delivery Is (and Why It Is Used)
Obstetric forceps are a paired, curved instrument designed to cradle the baby’s head and assist with guiding the baby through the birth canal during a vaginal birth. Think of forceps as a traction and positioning tool. When used appropriately by a trained clinician, forceps can shorten the second stage of labor and help avoid an emergency cesarean section in specific circumstances.
Forceps may be considered when one or more of the following applies:
- Prolonged second stage of labor, where pushing is not progressing.
- Non-reassuring fetal status, meaning there are concerns about the baby’s tolerance of labor.
- Maternal exhaustion or medical conditions where prolonged pushing is not advisable (for example, certain cardiac or neurologic conditions).
- Malposition, when the baby’s head position needs assistance to rotate or align for delivery.
A forceps delivery is typically attempted only when prerequisites are met, such as full cervical dilation, ruptured membranes, an engaged fetal head, an assessment of fetal position, and the ability to proceed to a cesarean if necessary. These prerequisites matter because they directly affect risk of forceps injury to a baby.
What “Forceps Birth Injury” Means
A forceps birth injury is any injury to the baby (and sometimes to the mother) associated with the use of forceps during delivery. Importantly, not every visible mark is an injury in the lasting sense. Many babies have short-lived bruising or swelling that resolves without long-term effects.
When parents use the term “forceps injury,” they usually mean one of three categories:
- Superficial soft tissue effects: bruises, abrasions, swelling.
- Nerve or muscle injuries: facial nerve palsy, brachial plexus injury, neck muscle injury.
- Serious internal injuries (rare, but urgent): skull fracture, intracranial hemorrhage, significant bleeding beneath scalp layers.
A clinically helpful approach is to separate common and temporary findings from red-flag findings that require urgent assessment.
Common, Usually Temporary Findings After Forceps Delivery
Many newborn findings after an assisted delivery are expected, monitored, and self-limited. These can still be upsetting to see, but they often improve quickly.
Bruising and superficial marks
- Bruising on cheeks, temples, or scalp.
- Small abrasions where the instrument contacted skin.
- Swelling that improves over days.
What parents can do: Ask the care team to document the location and size of marks, and ask when you should expect improvement. Photographing visible findings daily for a few days can help you track changes accurately.
Caput succedaneum and molding
- Caput succedaneum is swelling of the scalp tissue.
- Molding is temporary shaping of the head from pressure during birth.
These usually resolve over the first week or two.
Cephalohematoma (a special mention)
A cephalohematoma is a collection of blood beneath the periosteum (a layer covering the skull bone). It feels like a firm bump and does not cross suture lines.
Most cephalohematomas resolve over weeks. They can, however, increase the risk of newborn jaundice because the body breaks down the accumulated blood.
Ask about: bilirubin monitoring, follow-up timing, and warning signs of worsening jaundice (yellowing of skin/eyes, poor feeding, increased sleepiness).
If your child suffered a forceps birth injury, and you suspect Forceps delivery medical malpractice, call Nashville forceps delivery complications lawyer Timothy L. Miles today to see if you qualify for a forceps delivery complications lawsuit, and potentially entitled to substandial compensation. The call is free and so the fee unless we win or settle you case so call today and and see what a Nashville forceps delivery complications lawyer can do for you. (855) 846-6538 or [email protected].
Injuries More Strongly Associated With Forceps (What They Look Like)
Not all of these injuries are caused solely by forceps, because complicated labors have overlapping risks. Still, these are the conditions clinicians consider carefully when forceps were used.
1) Facial nerve palsy
Facial nerve palsy can occur if the facial nerve is compressed, leading to weakness on one side of the face.
Signs you may notice:
- Uneven crying (one corner of the mouth does not move).
- One eyelid may not close fully.
- Flattened nasolabial fold on one side.
Typical course: Many cases improve over weeks, sometimes months, depending on severity.
Practical care questions:
- Does the eye need protection (lubricating drops or taping guidance)?
- Should we see pediatrics, neurology, or ENT?
- When should improvement be expected?
2) Skull fracture or intracranial injury (rare, urgent)
These are uncommon, but clinicians take them seriously.
Potential signs:
- Seizure-like activity.
- Significant lethargy, poor responsiveness.
- Abnormal tone, apnea episodes, persistent vomiting.
- A rapidly enlarging head swelling or concerning head exam.
If any of these are present, evaluation may include imaging such as cranial ultrasound, CT, or MRI, depending on clinical urgency and local practice.
3) Subgaleal hemorrhage (rare, emergent)
Subgaleal hemorrhage is bleeding into the potential space beneath the scalp aponeurosis. It can be life-threatening because it may involve significant blood loss.
Signs include:
- Diffuse, boggy scalp swelling that can spread.
- Pallor, rapid heart rate, poor perfusion.
- Falling hematocrit or signs of shock.
This is an emergency requiring immediate neonatal care.
4) Brachial plexus injury (less directly tied to forceps, but may coexist)
A brachial plexus injury affects nerves controlling the arm and shoulder.
Signs:
- One arm is less mobile.
- Asymmetric Moro reflex.
- Arm held in an unusual posture.
Early assessment and, when indicated, early referral to a specialized brachial plexus team can improve functional outcomes.
5) Neck muscle injury and torticollis
Some babies develop torticollis (tightness in the sternocleidomastoid muscle), leading to a head tilt preference.
Signs:
- Preference to turn head to one side.
- Difficulty feeding on one breast or bottle angle issues.
- Flattening of one side of the head over time (positional plagiocephaly).
Early pediatric physical therapy is often very effective.
A Parent-Friendly Symptom Checklist (When to Seek Help)
Use this section as a practical reference. When in doubt, trust your instincts and contact your baby’s clinician or seek urgent care.
Seek urgent evaluation today if your baby has:
- Seizure-like movements, staring spells with unresponsiveness, or repeated jitteriness that does not stop when comforted.
- Trouble breathing, bluish color, repeated apnea, or persistent grunting.
- Poor feeding with dehydration signs (very few wet diapers, dry mouth, sunken soft spot).
- Marked sleepiness, difficult to arouse for feeds, or a sudden change in responsiveness.
- Rapidly increasing scalp swelling, especially if it feels boggy and spreads.
- Fever in a young newborn (follow your local guidance, but fever in early infancy is typically urgent).
Request a focused exam soon if you notice:
- Uneven facial movement when crying.
- One eye that does not close fully.
- One arm that moves less than the other.
- Persistent head tilt or strong head-turn preference.
- Worsening jaundice or jaundice that spreads to the legs.
How Clinicians Evaluate a Suspected Forceps-Related Injury
Evaluation is driven by the baby’s appearance, vital signs, neurologic exam, feeding, and the specific finding.
Common elements include:
- Newborn physical and neurologic examination repeated over time, not only once.
- Bilirubin checks if bruising or cephalohematoma is present.
- Hematocrit/hemoglobin if there is concern for bleeding.
Imaging when red flags appear
- Cranial ultrasound (often first-line in some settings for intracranial assessment).
- CT (rapid evaluation in urgent scenarios, balanced against radiation considerations).
- MRI (detailed assessment when the baby is stable and more detail is needed).
A constructive question to ask is: “What specific diagnosis are we ruling in or ruling out, and what findings would change management today?” This keeps communication precise and outcome-focused.
Treatment and Follow-Up: What Care Often Looks Like in 2026
In 2026, the most effective approach remains consistent: early recognition, structured follow-up, and targeted referral. The difference is that many hospitals now use more standardized pathways for newborn head trauma risk, jaundice monitoring, and early therapy referral.
Typical management by condition
- Superficial bruising/swelling: observation, jaundice monitoring, routine follow-up.
- Cephalohematoma: observation, bilirubin monitoring, parent education. Aspiration is generally avoided due to infection risk unless specifically indicated.
- Facial nerve palsy: observation, eye protection if needed, follow-up examinations, referral if not improving.
- Torticollis: pediatric PT, repositioning strategies (which could include specific techniques for managing head positioning), and monitoring head shape.
- Brachial plexus injury: early PT and prompt referral to a multidisciplinary team if weakness persists.
Why early therapy matters
For nerve and muscle conditions, time is function. Early physical therapy does not only treat range of motion. It also prevents secondary complications, improves symmetry, and supports feeding and positioning.
Feeding, Sleep, and Comfort: Practical Guidance for the First Weeks
If your baby has facial weakness, head preference, or discomfort, daily routines can feel more complicated. A few clinically grounded strategies can help:
- Feeding positions: If facial asymmetry affects latch or seal, ask for a lactation consultant and consider paced bottle feeding techniques when needed. Document which positions work best.
- Eye care: If an eyelid does not close fully, ask for clear instructions. Corneal protection can prevent avoidable complications.
- Position changes: Alternate head positions during supervised awake time to reduce head flattening and support neck mobility.
- Track patterns: Keep notes on feeds, diapers, alertness, and any unusual movements. This record helps clinicians detect trends quickly.
In some cases where there are significant health issues or complications arising from the conditions mentioned above, it may be necessary to explore legal options such as filing a lawsuit related to medical devices like Dexcom. If you find yourself in such a situation in 2026, you might want to see if you qualify for a Dexcom lawsuit.
Documentation: What Parents Should Request (Calmly and Clearly)
When forceps delivery complications occue and a concern arises, documentation serves two purposes: it improves continuity of care and it reduces confusion later.
Consider requesting:
Delivery Note and Operative Vaginal Delivery Documentation
- Indication for forceps.
- Type of forceps used (if documented).
- Number of pulls and duration of attempt (if recorded).
- Fetal station and position at application.
- Any complications noted.
Additional Records to Request
- The baby’s newborn exam findings and nursery or NICU notes.
- Any imaging reports, bilirubin trends, and discharge instructions.
You are not requesting these documents to escalate conflict. You are requesting them to ensure clarity, continuity, and proactive follow-up.
If your child suffered a forceps birth injury, and you suspect Forceps delivery medical malpractice, call Nashville forceps delivery complications lawyer Timothy L. Miles today to see if you qualify for a forceps delivery complications lawsuit, and potentially entitled to substandial compensation. The call is free and so the fee unless we win or settle you case so call today and and see what a Nashville forceps delivery complications lawyer can do for you. (855) 846-6538 or [email protected].
Long-Term Outlook: What Most Families Can Expect
Most babies delivered with forceps do well, and most visible marks resolve. When a more significant forceps delivery complications, outcomes vary by diagnosis and severity, but two themes consistently improve prognosis:
- Early identification of neurologic, muscular, or bleeding complications.
- Early intervention through pediatrics, therapy, and appropriate specialists.
Follow-up milestones to consider
Ask your pediatrician about a structured plan that includes:
- Early newborn follow-up within days of discharge (especially if bruising or jaundice risk is present).
- Re-check of facial movement, limb symmetry, and head/neck mobility at routine visits.
- Developmental surveillance and referral if milestones lag in motor skills, feeding, or coordination.
In parallel, trust the basics. If your baby feeds well, wakes appropriately, gains weight, and shows improving symmetry, those are meaningful indicators.
Prevention and Risk Reduction: What Matters Before and During Delivery
Parents do not control whether forceps are offered, but you can reduce uncertainty by discussing decision-making before labor, particularly if you have risk factors for forceps delivery complications.
Topics to discuss with your obstetric team in advance:
- Assisted vaginal delivery options: forceps vs vacuum, clinician experience, and typical scenarios for each.
- Thresholds for intervention: how fetal monitoring showing signs of fetal distress,labor progress are used to decide next steps.
- Escalation plan: when a cesarean would be recommended instead of continuing attempts.
- Pain management and positioning: optimizing pushing effectiveness and reducing fatigue.
- Communication commitments: asking for clear language during urgent moments, including a short explanation of indication, benefits, and material risks.
Proactive planning does not eliminate risf of a forceps birth injury. It reduces surprises and supports informed, timely decisions.
When Parents Consider Legal Advice (A Neutral, Practical Perspective)
Some families seek legal counsel after a serious forceps birth injury, particularly if they suspect Forceps Delivery Medical Malpractice. .Others do not, even when outcomes are significant. A neutral, practical approach is to separate emotion from action:
- If your baby has a confirmed significant forceps birth injury, it is reasonable to request a complete copy of records and seek a second medical opinion on diagnosis, prognosis, and care plan.
- If you are considering legal advice, look for counsel experienced in birth injury medicine and documentation, and focus on objective questions: Were prerequisites met? Was the chosen method consistent with clinical standards? Was fetal status monitored and acted upon appropriately? Was neonatal assessment timely and complete?
Regardless of your path, your child’s care plan and early interventions remain the priority.
To Do Today
If your baby was delivered with forceps and you are worried about the improper use of forceps during birth, a structured plan reduces anxiety and improves outcomes:
- Schedule prompt pediatric follow-up if not already arranged, ideally within a few days of discharge or baby showing signs of being injured during forceps delivery.
- Bring a written list of what you observed, including photos and timestamps or anything showing signs of fetal distress.
- Ask for a focused exam of head/scalp, facial movement, arms, and neck range of motion.
- Confirm bilirubin monitoring if bruising or cephalohematoma is present.
- Request referrals early if you see facial weakness, arm asymmetry, or head tilt preference.
Repetition for emphasis matters here: early recognition, early follow-up, early intervention.
Closing Perspective
A forceps delivery is often performed to achieve a safer, faster birth when time and physiology matter. If your baby has signs of forceps birth injury, you deserve clear explanations, a careful examination, and a proactive follow-up plan. Most issues resolve. Some require therapy and specialist care. All require that you are heard, that you are informed, and that your baby is monitored with precision.
If you want, share what you are seeing (for example: bruising location, any facial asymmetry, feeding issues, or head swelling timeline), and I can help you prepare a concise question list for your pediatric visit.
If your child suffered a forceps birth injury, and you suspect Forceps delivery medical malpractice, call Nashville forceps delivery complications lawyer Timothy L. Miles today to see if you qualify for a forceps delivery complications lawsuit, and potentially entitled to substandial compensation. The call is free and so the fee unless we win or settle you case so call today and and see what a Nashville forceps delivery complications lawyer can do for you. (855) 846-6538 or [email protected].
Frequently Asked Questions about a Forceps Birth Injury
What is a forceps delivery and when is it typically used?
A forceps delivery involves the use of obstetric forceps, which are paired, curved instruments designed to cradle the baby’s head and assist in guiding the baby through the birth canal during vaginal birth. Forceps are typically used to shorten the second stage of labor or avoid an emergency cesarean section in cases such as prolonged pushing, non-reassuring fetal status, maternal exhaustion or medical conditions, and malposition of the baby’s head.
What are common, temporary findings after a forceps birth injury?
Common findings of a a forceps birth injury include bruising on the cheeks, temples, or scalp; small abrasions where the instrument contacted skin; swelling that usually improves over days; caput succedaneum (scalp swelling); molding (temporary shaping of the head); and cephalohematoma, which is a firm bump due to blood collection beneath the skull’s periosteum. These signs generally resolve within days to weeks without long-term effects unless Forceps delivery medical malpractice was involved.
What is a cephalohematoma and what should parents watch for?
A cephalohematoma is a collection of blood beneath the periosteum of a skull bone that does not cross suture lines as a result of forceps delivery complications. It feels like a firm bump and typically resolves over weeks. Parents should be aware that it can increase the risk of newborn jaundice due to blood breakdown. Monitoring bilirubin levels, following up with healthcare providers, and watching for signs like yellowing skin or eyes, poor feeding, or increased sleepiness are important.
What types of injuries are more strongly associated with forceps birth delivery?
Injuries more commonly linked to forceps use include facial nerve palsy—characterized by weakness on one side of the face such as uneven crying or inability to close one eyelid—and rare but serious internal injuries like skull fractures or intracranial hemorrhage. These require careful clinical assessment and sometimes imaging studies.
How can parents advocate effectively for their child after a forceps birth delivery?
Parents can advocate by asking clinicians to document any visible marks or concerns thoroughly, photographing changes over time to track healing, inquiring about expected recovery timelines, understanding warning signs that require urgent evaluation (such as seizures or abnormal lethargy), and ensuring appropriate follow-up care with pediatricians or specialists as needed.
When should urgent medical attention be sought after a forceps birth delivery?
Urgent evaluation is necessary if serious signs of a forceps birth injury such as seizure-like activity, significant lethargy or poor responsiveness, abnormal muscle tone, apnea episodes, persistent vomiting, or rapidly enlarging head swelling occur. These symptoms may indicate serious internal injuries like skull fractures or intracranial hemorrhage requiring immediate imaging and treatment.